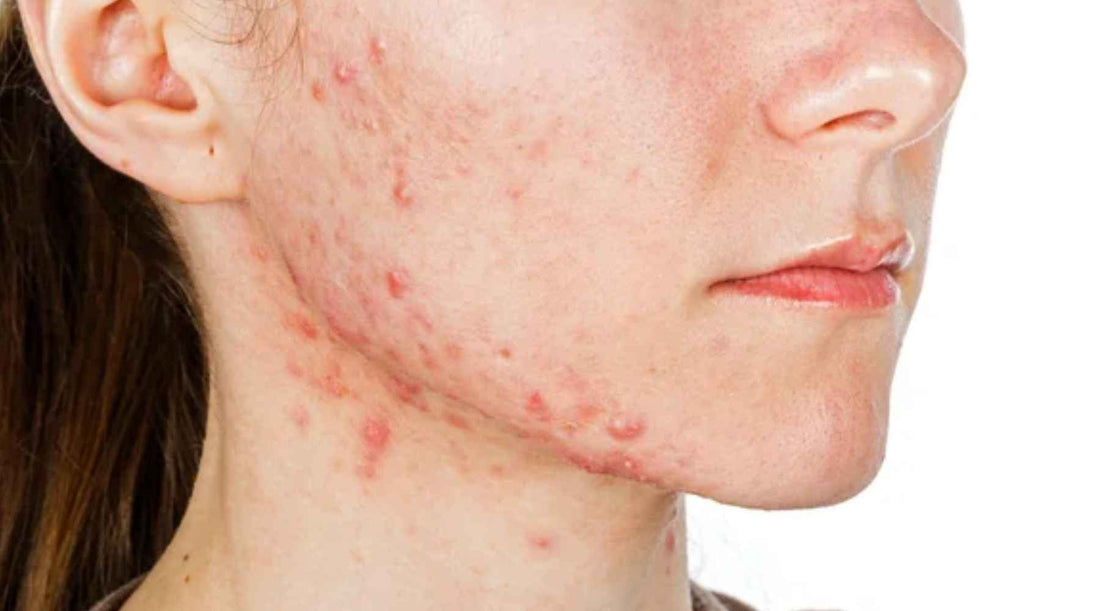
Acne is a common skin condition that affects millions worldwide, but among its various forms, cystic acne stands out as one of the most severe and challenging types to manage. Characterized by deep, inflamed lesions beneath the skin's surface, cystic acne can be painful, persistent, and detrimental to one's self-esteem. In this comprehensive guide, we delve into the primary treatment methods, causes, and preventive measures for combating cystic acne.
Understanding Cystic Acne
Cystic acne manifests as large, pus-filled cysts that develop deep within the skin. Unlike typical pimples, which surface relatively quickly and respond well to topical treatments, cystic acne lesions linger for weeks or even months and often leave behind stubborn scars. These cysts can occur anywhere on the body but are most commonly found on the face, chest, and back.
What Causes Cystic Acne?
Several factors contribute to the development of cystic acne. Hormonal fluctuations, particularly during puberty, menstruation, and pregnancy, play a significant role in triggering excess oil production in the skin's sebaceous glands. This excess oil, along with dead skin cells and bacteria, can clog hair follicles and lead to the formation of cystic lesions.
Genetics also play a crucial role in predisposing individuals to cystic acne. Those with a family history of severe acne are more likely to experience similar skin issues themselves.
Primary Treatments for Cystic Acne
1. Topical Treatments
While traditional over-the-counter acne products may not be effective for cystic acne, prescription-strength topical medications containing ingredients like retinoids, benzoyl peroxide, or antibiotics can help reduce inflammation and prevent new breakouts.
2.Oral Medications
In cases of severe cystic acne, dermatologists may prescribe oral medications such as isotretinoin (Accutane) or oral antibiotics to address inflammation, kill bacteria, and regulate oil production. These medications typically require close monitoring due to potential side effects.
3. Intralesional Injections
Dermatologists may administer corticosteroid injections directly into cystic lesions to reduce inflammation and promote healing. This approach can provide rapid relief from pain and swelling associated with large cysts.
4. Lifestyle Modifications
Adopting a skincare routine tailored to acne-prone skin and making healthy lifestyle choices can complement medical treatments for cystic acne. Practices such as gentle cleansing, avoiding harsh skincare products, and managing stress levels can help minimize flare-ups.
5.Professional Procedures
In some cases, dermatological procedures like chemical peels, microdermabrasion, or laser therapy may be recommended to improve skin texture, reduce scarring, and prevent future breakouts.
How Do I Stop Getting Cystic Acne?
While not all cases of cystic acne can be prevented, adopting certain habits can help minimize the risk of flare-ups:
- Maintain a Consistent Skincare Routine: Cleanse the skin gently twice daily, using non-comedogenic products suitable for acne-prone skin.
- Avoid Touching or Picking at Lesions: Manipulating cystic acne lesions can worsen inflammation and increase the risk of scarring.
- Stay Hydrated and Eat a Balanced Diet: Drinking plenty of water and consuming a diet rich in fruits, vegetables, and whole grains can support overall skin health.
- Manage Stress Levels: Chronic stress can exacerbate hormonal imbalances and contribute to acne flare-ups. Engage in stress-reducing activities such as exercise, meditation, or hobbies.
Cystic acne presents unique challenges and requires a multifaceted approach to treatment and prevention. By understanding the underlying causes, exploring primary treatment options, and implementing preventive measures, individuals can take proactive steps towards achieving clearer, healthier skin. Remember, consulting with a dermatologist is essential for developing a personalized acne management plan tailored to your specific needs and skin type. With patience, consistency, and professional guidance, conquering cystic acne is within reach.